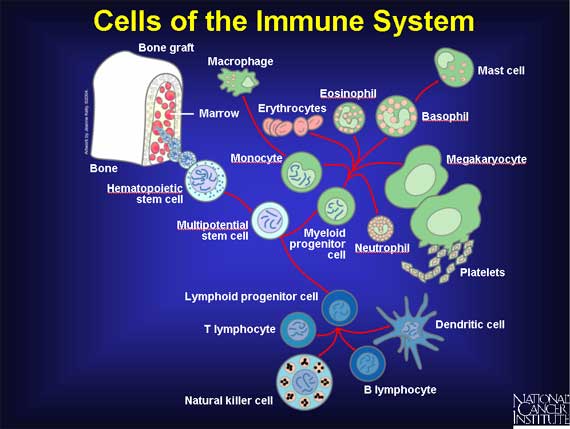
A couple of articles ago, I started writing an article on the flu, and it sort of expanded until it got to where it included vaccines and the human immune system, which is way too much stuff for one article. The immune system is way too cool (and involved) to just jam in between other topics, so I’m going to give over this article to the immune system. I’ll talk about the flu next time.
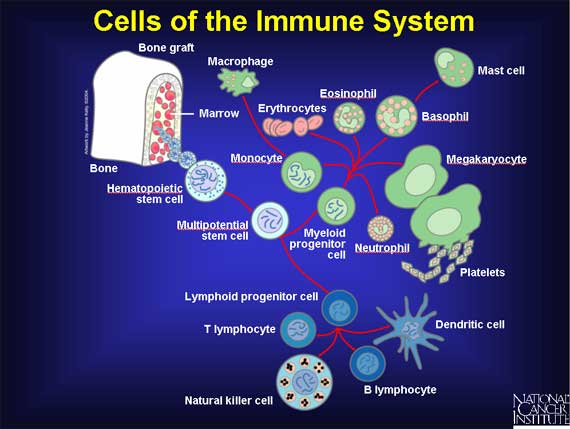
Source: National Institutes of Health, National Cancer Institute
All of Physiology is a magnificent interplay between Biology, Chemistry, Physics and Anatomy. The immune system is, perhaps, one of the best examples of how many different processes and many different organs and organ systems work together for various physiological purposes; in this case, to protect the body from infection. Before we get into the details, we need to define a few terms. An infection is when a microorganism, like a bacterium or virus, that can cause disease finds a place in a host (like a human) where it can live and multiply. I’ve mentioned in other articles that the human body is normally host to a vast array of microorganisms. They rarely make us sick and, in many cases (like the bacteria that live in our intestines), are necessary for normal function. They don’t usually make us sick for two main reasons. One is that most microorganisms are not pathogenic, which is to say that they are not potentially disease-causing. The other is that, even potentially pathogenic microorganisms can only cause disease if they gain access to places in or on the body where they can multiply to the point where they cause disease. Our skin, for instance, almost always has bacteria like Staphylococcus on it. As long as those bacteria stay on the surface, they rarely cause trouble. It’s only when they gain access to the interior, like through a wound, that they find a place where they can really start to multiply and cause problems.
The trick then is to make sure no potential pathogens find their way to places in the body where they can become established, multiply, and begin to do whatever it is that they do that damages our cells or interferes with our biochemistry, which is, ultimately, what makes us sick. To prevent that from happening, we have several lines of defense. The first line of defense is called “physical barriers”, and they are, by far, the most effective mechanism for keeping us healthy. Our skin is the primary physical barrier. It keeps the outside out and the inside in. We come into contact with untold millions of potential pathogens every day, and an intact skin is very effective at keeping them from infecting us. When you do something to open an hole in the skin, like cutting your finger, you break that barrier, and give potential pathogens an opportunity to get inside where conditions are good for them to grow and cause infection. This is why it is a good idea to clean and disinfect any wounds you receive. You need to remove as many pathogens from the wound as possible (by washing) and then kill the rest (by using antiseptics, like peroxide). Your body will also react to the wound. First off, it will bleed, which is good for washing dirt and microorganisms out of the wound. Then the process of inflammation will start. When tissues are damaged, there is a whole cascade of events that follow that is designed to help control infection and allow the damage to heal. That process is inflammation. It is marked by four signs and symptoms. A sign, by the way, is something that an outside observer, like your doctor, can see or measure. A symptom, is something that is experienced by the patient. Inflammation is marked by swelling, redness and heat (all of which are signs) and pain (which is a symptom). We tend to always think of inflammation as something bad that needs to be prevented or treated, but the reality of inflammation is more nuanced than that. Inflammation is complicated, but let’s summarize by saying that it is something that happens in damaged tissues that helps prevent infection, removes the damaged cells and sets the stage for new tissue to grow and heal the wound. Acute inflammation, which is inflammation that happens quickly in damaged tissue and doesn’t last too long, is a good and necessary part of healing, even if it is uncomfortable. Chronic inflammation can be damaging to healthy tissues, as in the case of conditions like osteoarthritis.
Your skin also has a number of holes in it normally. Things like your mouth, your nose, and your eyes, among others, are all, essentially, holes in your skin that are potential pathways for pathogens to get inside. And they do. Constantly. You might, for instance, have noticed that you breathe a lot. It’s one of those things we have to do, but it also is a great way for microorganisms to enter the body. Our anatomy has provided some help to prevent microbes from getting in. Most of the normal “holes” in the skin are lined with what are called mucous membranes. Membranes are just thin layers of tissue. These tissues can serve several purposes, depending on where they are, but one of the functions of the mucous membranes in the respiratory tract is to secrete mucous, which as you are probably aware, is a thick, sticky fluid, often referred to by a charming term like “snot” or “phlegm”. This fluid is ideal for capturing microorganisms that you might breathe in, keeping them from getting into your lungs, where they could do some serious damage. Mucous membranes are also included in the physical barriers. Another example of physical barriers are the enzymes in your tears. Just the constant washing of your eyeballs by tears and blinking helps keep your eyes from getting infected. Stomach acid is another. Most microorganisms that can cause infections in humans prefer to live in the conditions normally found in the body (otherwise, they couldn’t live and multiply in us). They like a temperature around 98.6 degrees Fahrenheit (37 degrees Celsius). This is why one of the responses to an infection is usually a fever. When your body temperature goes up, the microorganisms causing the infection usually don’t grow as fast, giving the rest of your immune response more time to respond. Human pathogens also like a pH (pH is a measure of acidity) around 7.4, which is where pH is for most of the body. Most bacteria we ingest with our food are killed by contact with our stomach acid, which has a pH of about 2. Acid with a pH of 2, by the way, is strong enough to eat the paint off your car. Stomach acid is strong stuff. There are some other physical barriers, but these are the main ones. Let’s move on to the second line of defense.
We’ve already mentioned one aspect of the second line of defense, which is inflammation. What characterizes the second-line responses is that they are not specifically directed against a particular pathogen. Rather, they are directed against anything that doesn’t belong inside your body. One seriously cool aspect of immunity is that every single cell you have (with the exception of some blood cells) have markers on them that label them as uniquely yours and belonging in you. This allows your immune system to distinguish between “self” and “not self”. Your second line defenses attack everything that is “not self” and leaves everything labelled “self” alone. There are some occasions where this system breaks down and your immune system attacks your own cells. These are called autoimmune reactions and are responsible for diseases like type-1 diabetes and lupus. Anyway, any object, like a microorganism, that enters your body lacks the proper “self” markers and the non-specific second line defenses will attack them. White blood cells called macrophages are part of this response. They are present in many different tissues and in blood, and they recognize, attack and destroy any pathogens (because the pathogens lack the “self” markers) they come into contact with.
This response is quite powerful, and it protects us against many potential infections that make it past the first line defenses, but it is not nearly as powerful as the third line defenses, which are sometimes referred to as the specific immune response”. The specific immune response is the part of the overall response that we usually think of. It’s the part where antibodies, vaccines and other things like that may play a role.
When you are born, there are cells produced in your bone marrow that have the ability to recognize specific pathogens, which has always amazed me. You are born with a fair degree of specific immunity, thanks, mainly, to transfer of antibodies from the mother’s blood through the placenta during gestation. There will, for instance, be a cell that recognizes a specific strain of Staphylococcus aureus. There will be another one that recognizes a different strain. There are cells made that will recognize almost any possible pathogen that anyone in your ancestry has ever encountered. While all of these cells are produced in the bone marrow, some of them are released into the blood, in which they travel to a gland that sits up on the top of the heart like a little witch’s hat, called the thymus. Once in the thymus, the cells mature. These cells, present at birth, will stay with you for your whole life, each one ready to recognize the specific pathogen it was designed for. These cells are called T-cells. Others of the cells will stay in the bone marrow as they mature. They will be called B-cells. T-cells and B-cells are both part of your specific immune response (because they recognize and attack specific pathogens), but they work through different, complementary mechanisms. Your specific immune response is so powerful that it can destroy any infection you get, with just a couple of exceptions. One exception is infections that are in places where the B- and T-cells can’t go, like they brain. There is a barrier in the blood vessels of the brain that keep B- and T-cells from passing into brain tissue. This is one reason why central nervous system infections, like meningitis, can be so dangerous—the immune response is limited. The other exception is infections that you are genetically not able to recognize. This is what happened to many of the native peoples in the Americas when Europeans first arrived. Many diseases the Europeans carried, in particular smallpox, had never existed in the Americas so the natives had no B- or T-cells waiting to fight the pathogens, so they died in huge numbers. Smallpox played a much greater role in European conquest of the Americas than did guns.
But I digress. Your B- and T-cells (called sentinel cells) just hang out in your blood your whole life, until they encounter the specific pathogen that they match. Once they recognize the pathogen, they start to reproduce in huge numbers. B-cells produce protein markers called antibodies that match the pathogens. The antibodies then attach to the pathogens, marking them for destruction. There are several ways antibodies help kill off the pathogens, but the main one is that white blood cells see the antibodies and attack and destroy the pathogens they are attached to. T-cells work differently. When they see the specific pathogen they match, they also start to reproduce very fast, making millions of copies of the T-cell that recognizes the pathogen. These specific T-cells then move through the blood and directly attack and destroy pathogens. This specific response is hugely powerful. As I said, it will kill off any infection you are likely to get. The only problem is that, because a lot of things have to happen to activate the specific response, the specific response is a little slow to react to infections. Sometimes, whatever is causing the infection will cause so much damage, so quickly, that you will die before the specific response can cure you. Sometimes, your immune system is compromised by other diseases, like AIDS, which prevents your specific response from working. Sometimes your body is weakened from other causes and your immune response, along with everything else, is weakened to the point that you can’t mount an effective specific response.
One final amazing benefit of the specific immune response is that, once you fight off a particular infection, you will probably be immune to infection by that same pathogen for the rest of your life. Part of what happens after those first cells encounter the pathogen for the first time and begin to multiply is that they produce another class of B- or T-cell called memory cells. These memory cells are basically just like the original cells that first recognized the infection. The only difference is that, the first time you were exposed, there was only one, or maybe a very few, sentinel B- or T-cells waiting to recognize the pathogen, and it might take a while (several days) for the pathogen and the sentinel cell to meet up and activate the process. After you make the memory cells, there are now going to be thousands of sentinel cells against that particular pathogen, and your specific immune response will be activated almost immediately the next time you are exposed. In this case, the specific response will usually wipe out the pathogens before they ever even have a chance to start another infection.
Sometimes, we don’t maintain immunity for life, or even for very long. Some pathogens change, or mutate, rapidly, which can help them avoid the immune response. COVID was one of these. The flu virus is another. These fast-changing microbes can then infect us to cause disease again, regardless of previous exposure. Also, the source of your immunity can matter. The immunity produced by some vaccines, particularly those against certain viruses, can decline over time, requiring a “booster shot”. Vaccines generally don’t produce as spectacular of an immune response as being actually infected, so the immunity can wear off. The COVID vaccine and the tetanus, pertussis and diphtheria (Tdap) vaccine are prime examples of vaccines that require boosters. The COVID vaccine needs a booster for both reasons. One is that COVID-19 mutates very fast and the other is that the COVID vaccine is a different type of vaccine (based on mRNA), which does not produce the same long-term immunity as the traditional vaccines do.
Every time I think about the immune system, the more amazed I am by it. It is among the most elegant and magnificent of all Physiological processes.